Rural Health Transformation Funding will Follow the Evidence
The CMS Rural Health Transformation Program creates a major opportunity for every state, but it also introduces a new operating requirement: prove progress, document outcomes, and stay ready for compliance review.
Listen to this Article
The Shift from Funding Opportunity to Accountability Model
CMS’s Rural Health Transformation Program is no longer a theoretical opportunity. It is now a national implementation effort. CMS has announced awards to all 50 states under the $50 billion program, with first-year awards in 2026 averaging approximately $200 million and ranging from $147 million to $281 million. The program will allocate $10 billion each year from FY 2026 through FY 2030, with half distributed equally among approved states and half allocated based on factors such as rurality, state policy actions, and the strength and scale of proposed initiatives.
For states, rural providers, EMS agencies, public health leaders, and Mobile Integrated Health teams, the funding is significant. But the more important lesson may be structural: RHT is not simply an infusion of federal dollars. It is an accountability model. The program is built around commitments, milestones, checkpoints, reporting, and measurable outcomes. In practical terms, rural health transformation will depend not only on what a state plans to do, but on whether the state and its partners can document that work in a way CMS can evaluate.
That distinction matters. Federal grants have long included performance measurement and reporting requirements. Under 2 CFR Part 200, federal agencies are expected to communicate program goals, expected outcomes, indicators, targets, baseline data, and reporting requirements; recipients and subrecipients must monitor activities for compliance and performance expectations and relate accomplishments to award goals. What makes RHT especially important is that performance evidence is tied to a structured, multi-year funding model. Future budget periods are not merely administrative renewals; CMS will reassess progress and can adjust funding based on whether states meet checkpoints, milestones, and policy commitments.
Conditional Funding and the Need for Continuous Performance Tracking
The Notice of Funding Opportunity is explicit. For state policy action commitments, states may receive conditional points in early years, but if a commitment is not fulfilled by the required deadline, CMS states that points will decrease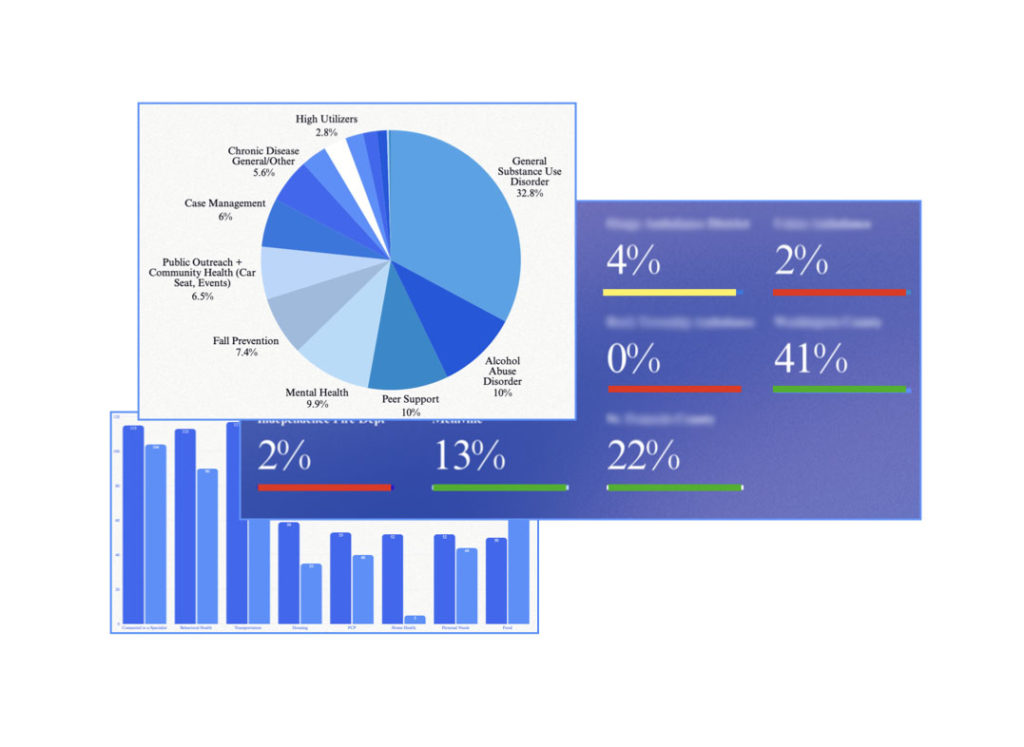 to zero for the related factor and that it will recover funds previously awarded based on that factor. For initiative-based funding, CMS uses an incremental scoring approach that assesses progress against milestones; the NOFO describes this allocation as inherently conditional on successful completion of the initiative.
to zero for the related factor and that it will recover funds previously awarded based on that factor. For initiative-based funding, CMS uses an incremental scoring approach that assesses progress against milestones; the NOFO describes this allocation as inherently conditional on successful completion of the initiative.
That creates a very different risk environment. A state may receive funding, begin implementation, subaward funds, contract with partners, and launch programs, only to face reduced future funding or recovery of funds if the documented progress does not match the commitments that supported the award. For state budgets and local implementation partners, this makes reporting infrastructure a core part of the program, not an afterthought.
CMS’s implementation guidance reinforces that point. In its April 2026 post-award FAQs, CMS states that future state budgets may go up or down depending on the state’s ability to meet RHTP checkpoints. The same guidance explains that initiative progress is assessed through a checkpoint model using supporting evidence, including milestone completion, metric reporting, and post-program planning. CMS also notes that changes to milestones, metrics, baselines, targets, or other scoring details must be reviewed and approved before they are final.
Building the Infrastructure to Measure and Deliver Outcomes
The reporting burden will also flow beyond state government. The NOFO allows states to subaward or subcontract RHT funds to partners such as universities, local health departments, provider associations, and other organizations, and it notes that federal award terms and conditions generally flow down to subawards and subrecipients. In practice, EMS agencies, MIH programs, hospitals, clinics, public health departments, behavioral health partners, and community-based organizations may all need to document their contribution to a state’s RHT goals.
Implementing and Sustaining Rural Health Transformation
This is especially relevant for Mobile Integrated Health and Community Paramedicine programs. MIH aligns closely with RHT priorities because it brings preventive care, chronic disease support, behavioral health coordination, care navigation, telehealth, and follow-up into the home and community. HealthCall describes MIH as a practical foundation for rural health transformation because it uses existing EMS and community resources, reduces transportation barriers, supports treatment in place and alternatives to transport, and creates measurable data around utilization and outcomes.
HealthCall also addresses one of the most difficult problems in statewide transformation: standardization without forcing every local program into the same workflow. In Florida, the Department of Health and HealthCall have partnered 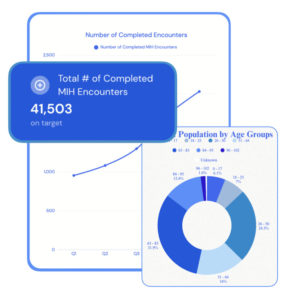 on standardized MIH data collection. The model allows individual EMS agencies to use workflows tailored to their communities while collecting state-required MIH data elements and translating records into a NEMSIS-compliant format for statewide analysis. HealthCall’s SMART Charts embed required data elements into local workflows, and state-relevant data can be gathered and submitted without extra re-entry steps.
on standardized MIH data collection. The model allows individual EMS agencies to use workflows tailored to their communities while collecting state-required MIH data elements and translating records into a NEMSIS-compliant format for statewide analysis. HealthCall’s SMART Charts embed required data elements into local workflows, and state-relevant data can be gathered and submitted without extra re-entry steps.
That type of infrastructure is exactly what RHT demands. States need local flexibility, but CMS needs comparable evidence. Local agencies need documentation that fits real care delivery, but state leaders need dashboards, exports, and audit-ready data. Programs need to prove both activity and impact: who was served, what was done, what changed, and how those changes relate to the state’s approved goals.
For states and local partners, the practical framework is straightforward:
Start with the outcome. Define the baseline, target, timeframe, geography, and data source before implementation begins.
Map every workflow to a measure. If a visit, referral, follow-up, assessment, or outreach effort supports an RHT milestone, it should be documented in a way that can be reported.
Manage lead measures continuously. Do not wait for annual reporting to discover a performance gap. Monitor referrals, encounters, task completion, follow-up closure, risk trends, protocol adherence, and patient engagement in real time.
Standardize what must be standardized. States need comparable data across counties, agencies, and partners. Local teams still need workflows that reflect the reality of their communities.
Prepare for audit and evidence review. Milestones, metrics, baselines, targets, budget changes, and scoring details should be traceable, explainable, and defensible.
